Postpartum Depression in Women The Illness Mothers Are Told to Ignore
Every year, millions of women give birth, and many are expected to adjust to motherhood quickly and quietly. For women experiencing postpartum depression, that expectation can make it harder to recognize that something is wrong. Postpartum depression in women is not the baby blues. It is a clinical illness that causes persistent sadness, anxiety, and emotional detachment.
In Pakistan, where up to 60% of new mothers are affected and nearly 90% go untreated, most mothers suffer without ever receiving a diagnosis.
What Is the Difference Between Baby Blues and Postpartum Depression?
The baby blues are real. In the first week or two after delivery, most women experience some emotional fragility. Mood dips, unexpected crying, a strange mix of love and overwhelm. This is the body adjusting to a steep hormonal drop, and it typically resolves on its own within two weeks.
Postpartum depression is a different illness entirely. It is deeper, more disruptive, and it does not fade with rest. It can develop within the first four weeks after birth or appear gradually across the first year. Baby blues vs postpartum depression is a distinction that matters because one passes, and the other requires treatment.
Recognizing the Symptoms Early
The challenge with postpartum depression symptoms is that early signs are easy to confuse with ordinary new-mother exhaustion. That confusion is exactly what allows it to go undetected for so long.
Common signs to watch for:
- Persistent low mood that does not lift after rest or time
- Extreme fatigue after childbirth, far beyond the exhaustion expected to care for a newborn
- Inability to bond with the baby or feeling emotionally detached
- Uncontrollable postpartum mood swings or sudden irritability
- Intense guilt, shame, or a deep sense of failure as a mother
- Postpartum anxiety symptoms, including intrusive thoughts and constant dread
- In severe cases, thoughts of self-harm or harm to the newborn
PPD does not always look like sadness. Some women appear composed on the outside while falling apart privately.
At the most severe end is postpartum psychosis, a rare but genuine psychiatric emergency involving hallucinations and rapidly shifting mental states that requires immediate medical attention.
Postpartum Anxiety: The Overlooked Side of Maternal Mental Health
Not all mothers experience postpartum depression as sadness. For many, it arrives as anxiety. Unlike general anxiety, postpartum anxiety is persistent, often irrational, and tied directly to the hormonal upheaval of new motherhood. A mother may feel convinced something terrible is about to happen to her baby, even when everything is fine.
In Pakistani women, this goes unrecognized for a specific reason. Worry about a newborn is expected, even celebrated as devotion. So when anxiety becomes clinical, the people around her see a good mother, not an unwell one. That cultural blind spot is a key reason perinatal mental health and women's health in Pakistani women remains so significantly underreported.
What Causes Postpartum Depression?
Biological Triggers
- Estrogen and progesterone drop steeply after delivery, disrupting mood regulation
- Thyroid issues postpartum can produce symptoms that closely resemble depression
- Hormonal shifts affect every woman differently, which is why onset and severity vary
- A history of depression or anxiety significantly raises the risk
- Sleep deprivation in the early weeks compounds the biological strain
Risk Factors
- A traumatic delivery or inadequate antenatal care
- Marital conflict or feeling unsupported by a partner
- Financial hardship or housing insecurity
- Stressful life events during the motherhood transition
- In Pakistani households, social pressure around the gender of the child
It is rarely one thing. It is the combination, layered on top of a body already pushed to its limits, that tips the balance.
Understanding the Postpartum Recovery Timeline
Recovery after childbirth is not linear, and emotional changes can shift significantly across the first year. Understanding where a mother is in that timeline helps identify when something needs attention.
- First 2 weeks: Emotional shifts are common and expected. This is the typical baby blues phase, driven by hormonal changes after birth.
- 1 to 3 months: Early signs of PPD may begin to appear, including fatigue after childbirth, social withdrawal, and persistent sadness.
- 3 to 12 months: Without support, symptoms can deepen considerably. Many women in Pakistan continue to struggle silently throughout this period.
- Beyond 1 year: Untreated postpartum depression can extend long-term and significantly impair overall maternal postpartum recovery.
How Long Does Postpartum Depression Last?
Without treatment, PPD can persist well beyond the first year. This is not a theoretical risk. Research tracking Pakistani women found postnatal depression rates increasing from 34% at three months to over 43% at twelve months after birth. That is not recovery. That is deterioration.
With appropriate care, most women see meaningful improvement. The postpartum recovery timeline varies by individual, but one consistent finding across the evidence is clear: the earlier it is caught, the better the outcome.
Why Pakistan's Numbers Are Alarming
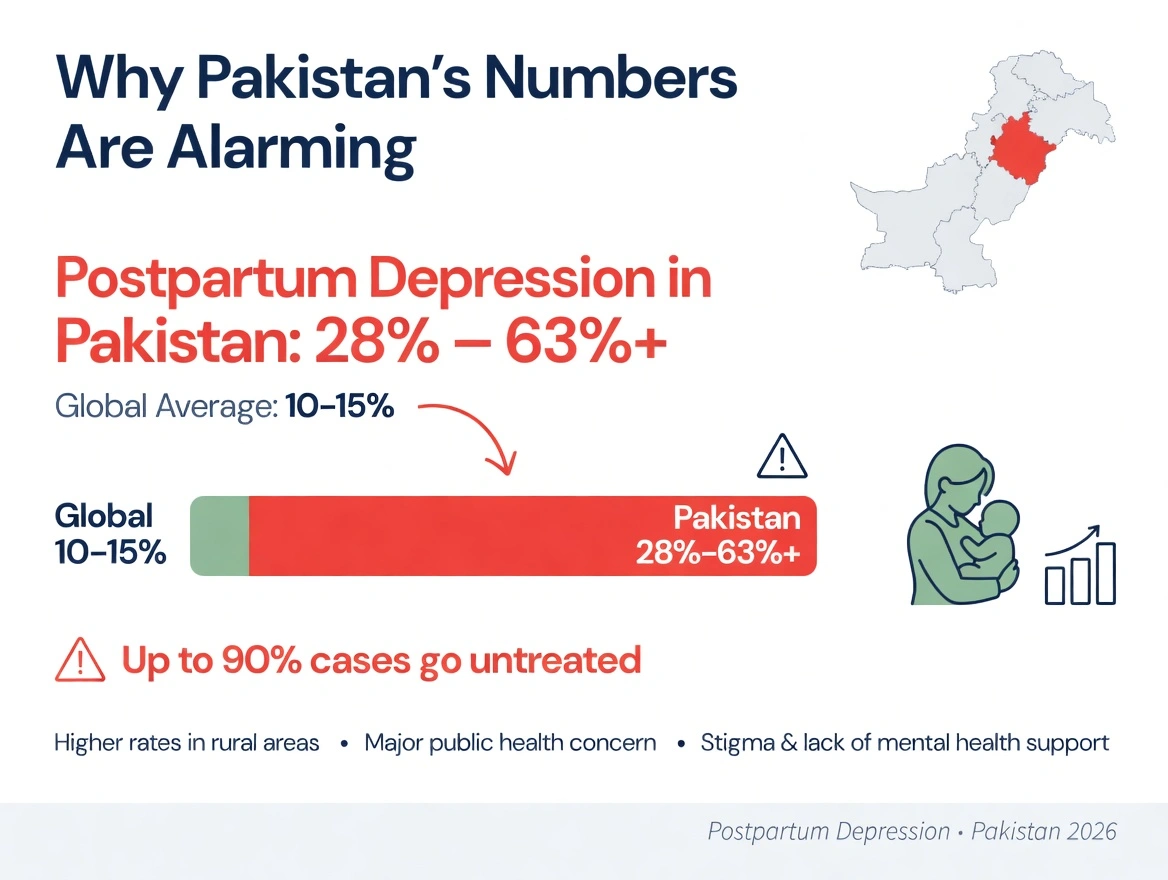
Studies from Pakistan have reported high rates of postpartum depression, with prevalence estimates varying widely across settings. Research places the figure between 28% and over 60%, nearly four times the global average. Yet up to 90% of affected women go undiagnosed and untreated. Women in rural communities often live hours from any functional facility, and seeking care requires transport money, lost wages, and frequently, permission from family members. Even at routine postpartum visits, mental health is almost never discussed.
The Culture of Dismissal
In many Pakistani households, a new mother's emotional state is simply not considered a medical concern. If she cries, she is tired. If she withdraws, she is ungrateful.
A study across healthcare institutions in Pakistan found that close to half of the social support systems surrounding new mothers, including husbands, mothers-in-law, and siblings, held negative attitudes toward PPD.
Untreated PPD disrupts early bonding, delays a child's development, and in the most serious cases, has contributed to maternal mortality.
What Treatment Looks Like
Postpartum depression is treatable, and recovery is possible with the right support. The approach depends on how severe the symptoms are, but options exist at every level, from professional therapy to everyday household changes.
Clinical Options
- Cognitive behavioral therapy is the most evidence-supported approach for new mothers
- Trained community health workers delivering psychosocial support have shown real outcomes where specialists are unavailable
- Antidepressants safe for breastfeeding are available, and a qualified clinician can guide that decision individually
Everyday Support That Makes a Difference
- Consistent rest and proper nutrition during recovery
- Reliable emotional support from a partner, family member, or peer
- Open, nonjudgmental dialogue within the household
Knowing when to seek help is important. If sadness, anxiety, or persistent emotional distress lasts more than two weeks after delivery, speak to a healthcare provider. Do not wait for it to pass.
Conclusion
With the right support and early intervention, recovery from postpartum depression is possible. Recognizing it early, speaking about it openly, and accessing the right care can change outcomes entirely.
SHINE Humanity has been working since 2009 to bring mental healthcare, community midwifery, and maternal support directly to underserved families across Sindh. Every mother who receives help is proof that maternal mental health Pakistan cannot remain an afterthought any longer.
Frequently Asked Questions
1. What is the difference between baby blues and postpartum depression?
Baby blues resolve within two weeks on their own, while postpartum depression is a clinical condition that persists and requires proper medical treatment.
2. How common is postpartum depression in Pakistan?
Prevalence ranges from 28% to over 60%, making Pakistan one of the most affected countries in Asia, with the majority of cases going untreated.
3. How long does postpartum depression last without treatment?
It can last months to years, with evidence showing depression rates in Pakistani mothers actually worsening across the first twelve months postpartum.
4. Can untreated postpartum depression affect the baby?
Yes, it can disrupt early bonding and has been linked to delays in a child's cognitive and emotional development.
5. When should a mother seek help after childbirth?
If emotional distress, sadness, or withdrawal persists beyond two weeks after delivery, speaking to a healthcare provider immediately is essential.
